Many hospitals participating in the Medicare BPCI Advanced program have recognized the importance of thorough coding of diagnoses to ensure that all applicable Hierarchal Condition Categories (HCC's) for each patient have been identified and coded on the Medicare bill. This is important because a significant component of the BPCI target is the Patient Case Mix Adjustment (PCMA) that utilizes an aggregation of each patient's HCC score in computing the overall target for an episode group. However, it's impossible to effectively target all 90,000 ICD 10 diagnosis codes for identification and coding, so focusing on a limited number of diagnoses that are likely to have the greatest effect on the BPCI Advanced target is a more cost-effective approach. A graphic of this process is shown below.
Filtering down the universe of ICD codes to those that are mapped to HCCs is the first step in this process. From about 90,000 ICD10 diagnoses, only about 10,000 are mapped to HCCs, so that smaller set of diagnoses is the initial focus for improving HCC coding. But wait – many of those diagnoses are already carefully evaluated by the hospital DRG groupers to maximize DRG weights – they are either used in determination of the DRG category itself or in the stratification of the DRG by presence of complications or major complications. Efforts at improving coding for these diagnoses are unlikely to be fruitful because they have already been subject to significant scrutiny. Because of this, focusing on other DRGs will increase the effectiveness of this process, and removing these diagnoses brings a list down to about 2500 diagnoses that are mapped to HCCs but are not used to determine DRGs.
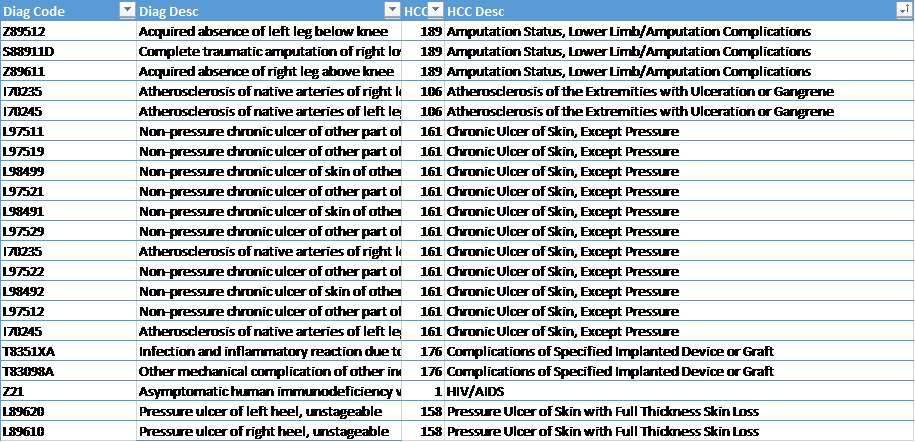
But a list of 2500 diagnoses codes is still too broad for a targeted effort, especially since some of these diagnoses may be rare or have a minimal contribution to the HCC score. To develop a more compact list of high-value diagnoses we filtered that list down to those that map to an HCC having a higher than average HCC risk factor, and then ranked that list by volume in a sample Medicare population. From that list we selected the top 25 diagnosis codes and their respective HCC categories, which are shown in the list below.
Notably, more than half of the high-volume, high-value diagnosis codes are related to chronic skin ulcers, indicating the importance of coding these diagnoses that won’t get picked up by the DRG coding editors but can be significant to BPCI Advanced targets. Others group into the clinical categories of amputation status, atherosclerosis, HIV, complications related to implanted devices, and pressure ulcers. This list may be a manageable size for clinician focus in documenting diagnoses in patients while providing the greatest potential increase in BPCI Advanced targets.
And here's where an analyst might believe that he has reached a useful conclusion, which is that coding pressure ulcers is a key to improving HCC scores in BPCI. But any knowledgeable clinician will know that pressure ulcers are the result of improper medical care and should be avoided as much as possible. Coding them is not a key to HCC improvement. So excluding pressure ulcers from the above list leaves few diagnoses that are critical to HCC assignment but aren't already being examined by the DRG coding editors. This suggests that an effort to improve coding of hospital claims specifically to improve HCC scores may not be worth the additional resources necessary for such an initiative. Most of the diagnoses that affect HCC assignment are already being reviewed by the DRG coding editors and further analysis may not be worth the effort.
